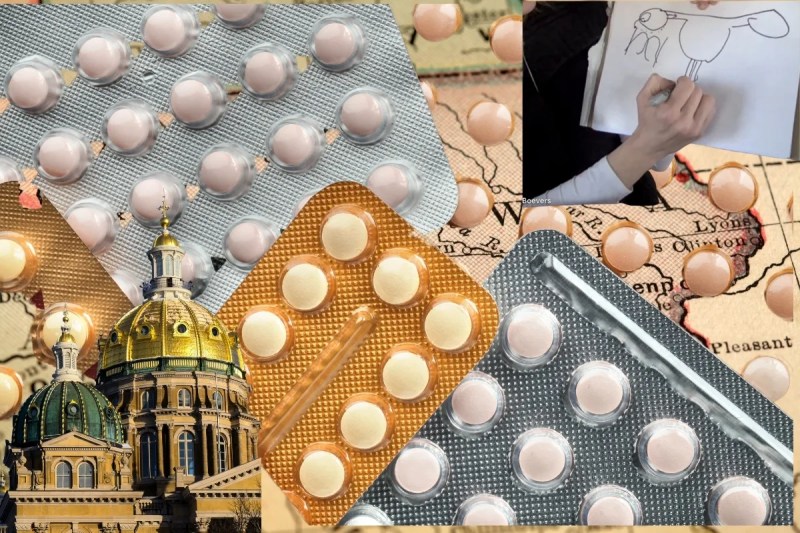
When Dr. Emily Boevers, an OB-GYN in Waverly, first sits down with patients for birth control consultations, she asks them a series of questions about why they want to use it, and for how long.
“The thing that I think is really important to keep in mind about birth control is that these are hormonal medications that actually treat a wide variety of symptoms for women,” she said.
Beyond preventing pregnancy, hormonal birth control methods like the pill can be used to regulate menstruation, lower the risk of some cancers, treat endometriosis, and improve symptoms of perimenopause—among others. Yet many people don’t have a basic understanding of how these medications work.
“More often than not, when I see people who are requesting consultation for contraception, it’s oftentimes because of painful or severe menstrual cycles or symptoms associated with those menstrual cycles,” she said.
Those symptoms—which can include debilitating cramps and heavy bleeding—can negatively impact patients’ quality of life, Boevers said.
“Preventing pregnancy is another really important reason. But these medications are very, very valuable as a woman’s health medication to help manage a lot of those symptoms of severe menses,” Boevers said.
Iowa lawmakers weigh in on contraceptives
Proposed legislation to make hormonal birth control available “over the counter”—without a prescription—has stalled in the Iowa Legislature, in part because of far-right conservative lobbyists and anti-abortion politicians.
That’s despite polling showing more than 3 in 4 Iowans support pharmacies selling over-the-counter birth control pills to people ages 18 and older. Even Gov. Kim Reynolds—an anti-abortion Republican whose term ends in 2026—made prescription-free birth control one of her legislative priorities.
Conservative religious groups and far-right Republicans in Iowa have raised unrealistic concerns about the safety of over-the-counter birth control pills. When presented with a bipartisan bill to legalize prescription-free birth control, Iowa House Republicans attached amendments to the legislation to make pharmacists treat birth control like abortion medication.
The two are not the same thing.
“There is no method of birth control that is the same or functions in the same way as abortion,” Boevers said.
Birth control is not an abortion
To put it simply: Birth control prevents pregnancy from happening, while an abortion ends a pregnancy that has already begun, Boevers said. (For more information about abortion, here’s a good resource.)
Pregnancy occurs when an egg is released from an ovary, becomes fertilized by a sperm (creating a zygote, a blastocyst, and then an embryo), and implants in the lining of the uterus.
Medically speaking, Boevers said, implantation is the key.
“There’s really no way to have that fertilized embryo develop in a way that a pregnancy develops without that final step of implantation occurring,” she said.
Between ovulation—when an egg is released from the ovaries—and implantation, Boevers said “there’s a lot of steps along the way where birth control methods can intervene to prevent pregnancy from occurring.”
Birth control types
In her consultations with patients, Boevers said the questions she asks can help her narrow down a patient’s birth control options to two or three they would like to try, based on their wants and needs.
All of those types boil down to a few strategies that work at different points in the reproductive cycle: preventing ovulation and/or preventing implantation.
Hormonal birth control like the pill, implants, injections, the patch, and the ring work to prevent ovulation, meaning no egg is released.
These forms use either a mix of estrogen and progestin—hormones the body makes naturally, and which regulate the ovulation cycle—or progestin alone.
Intrauterine devices (IUDs)—those with hormones and those without—work by affecting the way sperm move in a few ways. They also thicken the mucus in the bottom part of the uterus (the cervix), which prevents sperm from getting into the uterus in the first place.They can prevent ovulation.
IUDs are tiny t-shaped devices placed in the uterus, and they last for 3-12 years, depending on the brand. Some are made using non-hormonal copper, which slightly increases inflammation in the uterus enough to change the lining. Copper also changes the way sperm move.
The birth control implant has the same high effectiveness of an IUD (though all of the methods mentioned are effective more than 90% of the time). It’s a thin rod placed in the arm and releases progestin. It works for up to five years.
Emergency contraception (also known by brand-name Plan B) is birth control that can be taken within a few days of having unprotected sex.
Because there’s not always an egg, and because sperm can live in the reproductive system for up to five days, people who are not already on birth control can take emergency contraception to primarily prevent the release of an egg or prevent fertilization.
None of these birth control methods prevent sexually transmitted infections, though. So Boevers recommends using condoms or other barrier methods, too.
For a comprehensive rundown of the different types of contraception and their forms, Planned Parenthood has a useful guide on their website.
What about side effects?
No medicine is without any side effects, but birth control side effects generally aren’t dangerous. As with any medication, doctors and pharmacists can help screen patients avoid the types that might result in rare but serious side effects—like blood clots or cancer. Potential side effects are also listed on the packaging.
Boevers pointed out that Tylenol overuse can cause liver damage, but it’s something people are aware of and tolerate the risk for.
“At the level that these hormones are administered in your daily birth control pills, there are still those risks, but they are most pronounced in people who are already predisposed to them,” Boevers said. “Most of our hormonal contraceptive options at this point in time have a very low side effect profile.”
When hormonal birth control was first introduced, the levels of estrogen and progestin were much higher, which caused more side effects that were more severe. Nowadays, doctors and scientists have a better understanding of how much of the hormones it takes for the medication to be effective.
A new era of access to birth control
The first over-the-counter birth control pill approved in the US began online sales this month. The Opill is now available on Opill.com and through Amazon. It costs about $20 for one month, or $50 for a three-month supply.
It’s also available at pharmacies throughout the US—and for people in states without in-person, over-the-counter access, FDA approved contraceptives are now within reach.
Opill is an older class of contraceptive, sometimes called minipills, and only contain progestin, which generally leads to fewer side effects than the more popular combination estrogen and progestin pills.
“As an obstetrician gynecologist, I certainly support patients having access to birth control,” Boevers said. “I think over-the-counter birth control will only improve the rates of unintended pregnancies, so I think that’s a great win for our patients, particularly in a rural place like Iowa.”